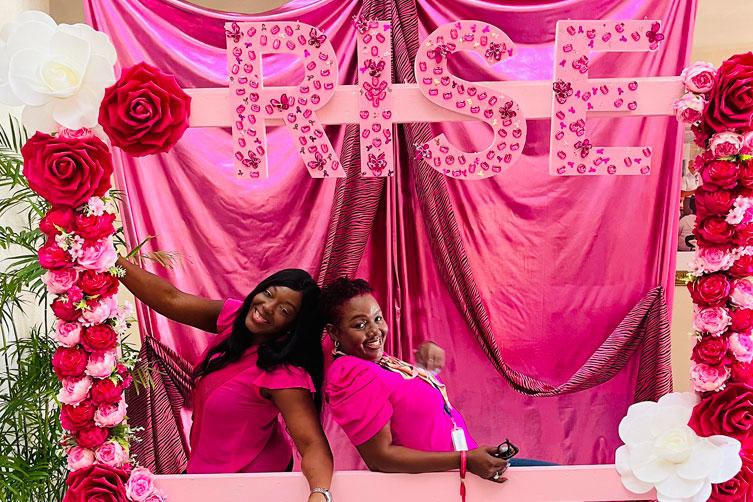Breadcrumb
- About Us
- News & Publications

AUC News and Publications
Search News Posts
343
Since earning his Doctor of Medicine (MD) degree at AUC, Dr. Stivala has also served as a reservist in the United States Army Medical Corps
Dr. Wesley Nilsson is an obstetrician gynecologist (OB/GYN) and board certified fellow of the American Congress of Obstetricians and Gynecologists (FACOG). He graduated from American University of the Caribbean School of Medicine (AUC) in 2017 — and hasn’t slowed down since.
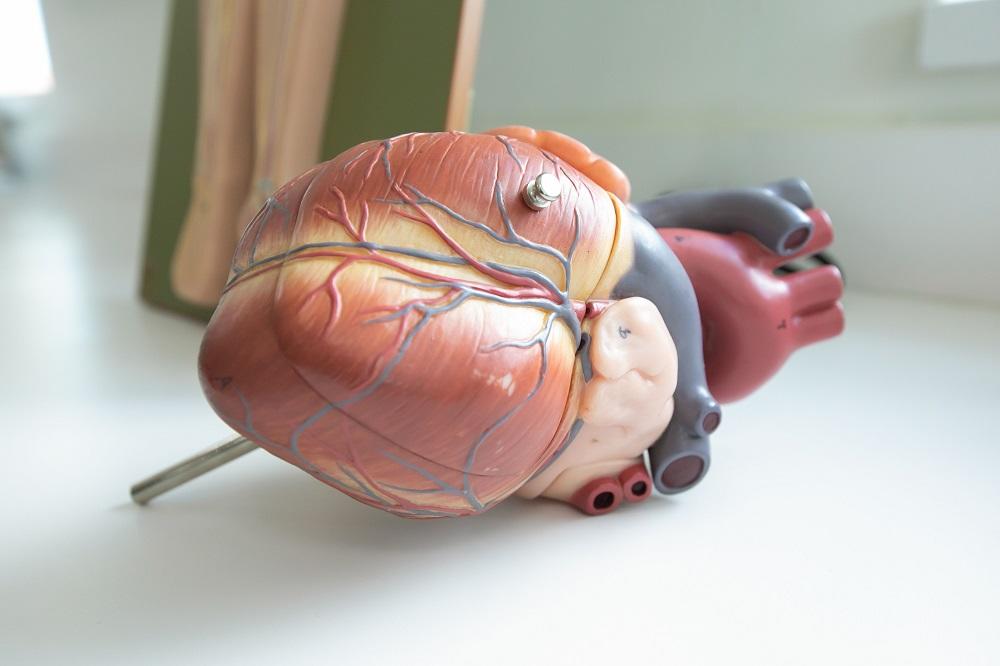
Today, at American University of the Caribbean School of Medicine (AUC), we are lucky enough to share the company of pediatric cardiologist and AUC alumna Annie Tedga, MD ’11.
In an effort to spread awareness and learn more about this disease, we sought the wisdom and advice of AUC grad Valerie Garden, MD ’89, an ophthalmologist and oculoplastic surgeon in Santa Rosa, California. We also sought her thoughts on National Women Physicians Day, which takes place February 3.
On the heels of Alzheimer's Awareness Month in November, we interviewed Izabella Shuvayev, MD ’13, a geriatric psychiatrist who specializes in Alzheimer's disease, dementia, and other cognitive and neurodegenerative disorders.
On December 1, World AIDS Day kicks off AIDS Awareness Month, a time to bring attention to this deadly disease, honor those who have been lost to it, and work to end the related stigmas. Acquired immunodeficiency syndrome (AIDS) is an advanced stage of human immunodeficiency virus (HIV), an infection that attacks the body’s immune system.
Dr. Christine Armstrong is an obstetrician-gynecologist in Connecticut. Dr. Shanique Ampiah is a pediatric psychiatrist in Florida. Different specialties. Different locations. Both share common ground when it comes to the mental health of moms.
At FemCare OB-GYN, an obstetrics and gynecology practice in Miami, a 29-year-old woman who recently arrived from Nicaragua was seeking help for severe abdominal pain. She had been suffering with it for months. She was desperate, distraught, and crying as she struggled in Spanish to voice her symptoms.
American University of the Caribbean School of Medicine (AUC) was a proud sponsor of Positive Foundation's Pink Walk, an annual event held in recognition of breast cancer survivors, warriors, and those who have lost the fight against breast cancer.
Pagination
- Previous page disabled ‹‹
- Current page 1
- Page 2
- Page 3
- Page 4
- Page 5
- …
- Next page ››
- Last page Last »

Still Have Questions? We Can Help
We're happy to answer any questions you might have during the application process.