Written by Shalom Adams, with photos by Tayler Avakian
In every semester at AUC, students take an Introduction to Clinical Medicine (ICM) class, which is designed to lay the foundation for developing clinical skills. You start by learning how to interact with your future patients—how to approach patient interviews with an open mind, and in turn, allow the patient to open up to you. Not only does this enable you, as a future physician, to learn key information needed to treat them, but it also helps build a trusting relationship between patient and physician.
In addition to learning these social skills to treat patients, we also practice physical assessments on a patient: going through each organ system of the body and developing the skills needed to evaluate each system. This helps us get more comfortable with the process of physical examinations, and prepares us to recognize both normal and abnormal findings.
So, you might ask yourself the following questions: When will I see my first patient where I have to make decisions for a real situation? Will I have to wait to learn those skills until after I take my USMLE Step 1 exam and start clinical rotations?
I personally thought I would have to wait until I stepped into a hospital—but that wasn’t the case.
Bringing Coursework to Life
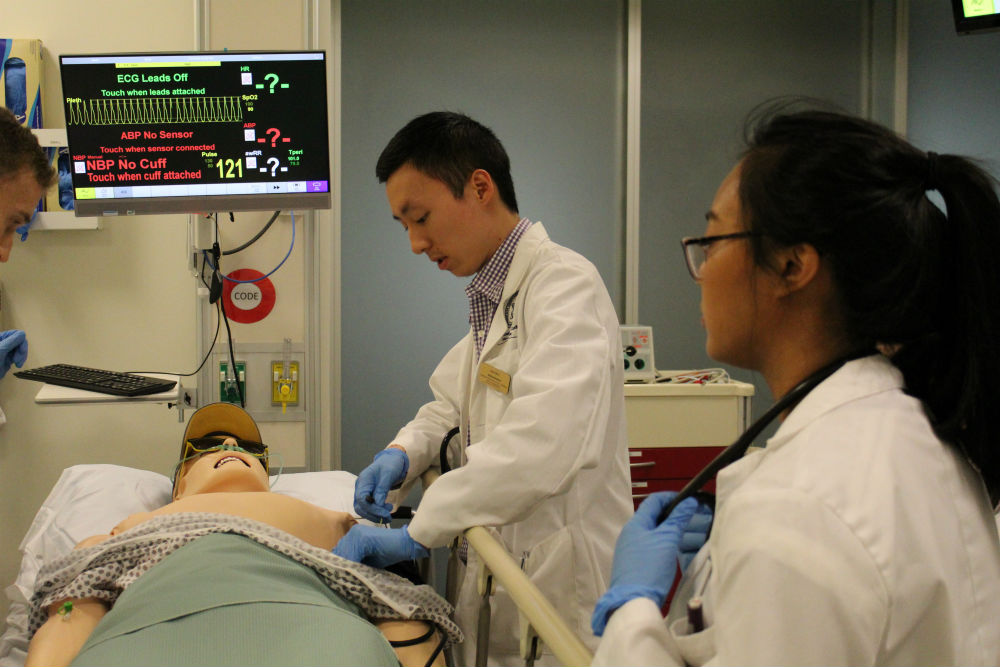
AUC has simulation centers that provide a hospital-like setting with standardized patients, which enables us to further hone our clinical skills. In the 3rd semester, we focus a lot more on diseases, so our first ICM workshop featured a patient with symptoms that we had learned about in class. I worked with a patient that integrated several concepts from pathology, physiology and medical microbiology.
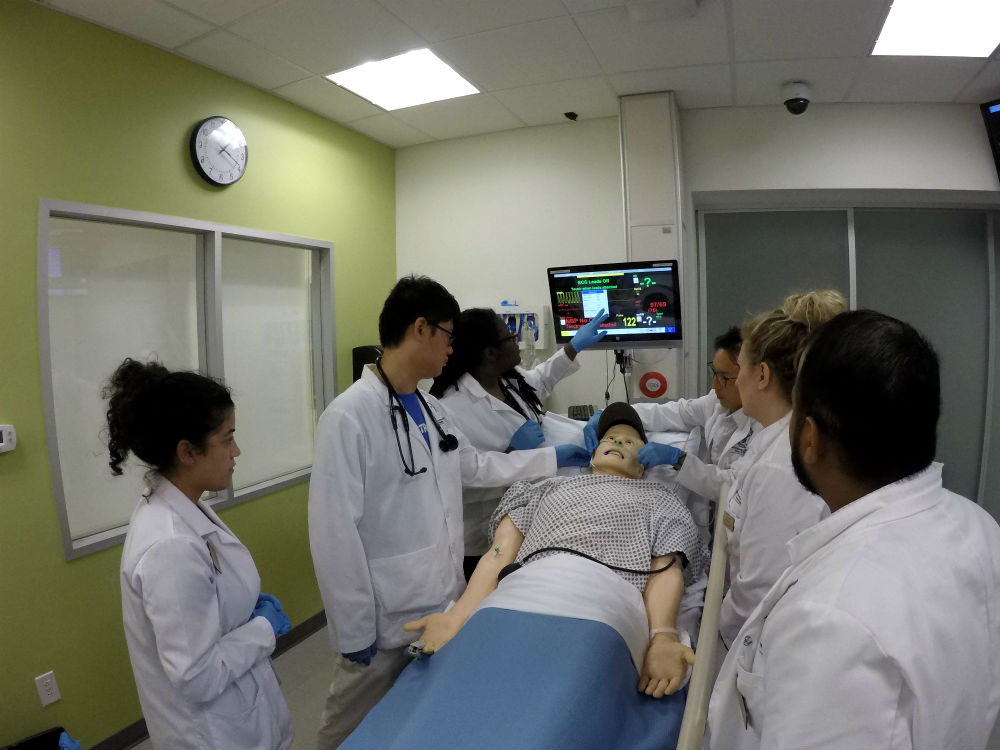
For this workshop, our class was split into groups of six students. This was to simulate a team of doctors seeing a patient. Each one of us was given a role: team leader, monitor, equipment manager, and two to lead the physical exam. The leader spoke to the patient (a simulation mannequin or model) first, asking why they had come into the hospital that day. While our team leader was talking to the patient, he was also instructing his team on what to do.
As a team, we would respond with treatment based on the symptoms of the patient and monitor reading. If the situation changed in the room for better or worse, we would re-evaluate and respond to the new situation. Everyone in the group reacted to the patient as if it were a real situation.
At the same time, a faculty member talked to us through the simulation model (he was listening and watching us from a different room) which allowed us to have a real conversation. The model has oxygen readings and all of the other monitors that patient would have in a hospital.

When our medical team entered the room and introduced ourselves, we attached the medical equipment to the model, and the reading came up on the monitor. As we got a chief complaint and a patient history, we reacted to the patient. In our setting, the patient had problems from all of our classes: presenting with a history of urinary tract infections, but with the main complaint of fever and dyspnea.
After conferring with our team about possible diagnoses, we met with all of our professors and the other groups doing the workshop. Each of our teachers got up to discuss the case with us and spoke about the diseases in a clinical setting. They went through the case thoroughly, reviewed our responses to the patient, interacted with us, and taught us about each aspect of the case as related to their respective subjects.
While it’s rare to frequently get a patient with all of these problems, it was the perfect way to integrate all of our classes. It opened our minds to how we should be viewing the subjects we learn separately as integrated into a clinical setting.
The Big Picture
After the scenario, our professor went around the room and asked each one of us what we had learned from the workshop. For me, it taught me the importance of a team. When you are there assessing the patient, it’s easy to view the patient through just one perspective of what condition they might have. But in a team setting, you’re able to share ideas with your colleagues and keep your mind open to see the big picture.
This workshop really helped me evaluate my learning style and become familiar with a clinical setting. Through this opportunity to experience a simulated case, I know I will be able to better understand diseases and synthesize my knowledge in the future. I look forward to 5th semester when AUC holds many more of these workshops to strengthen our skills.




